Warning: This is LONG.
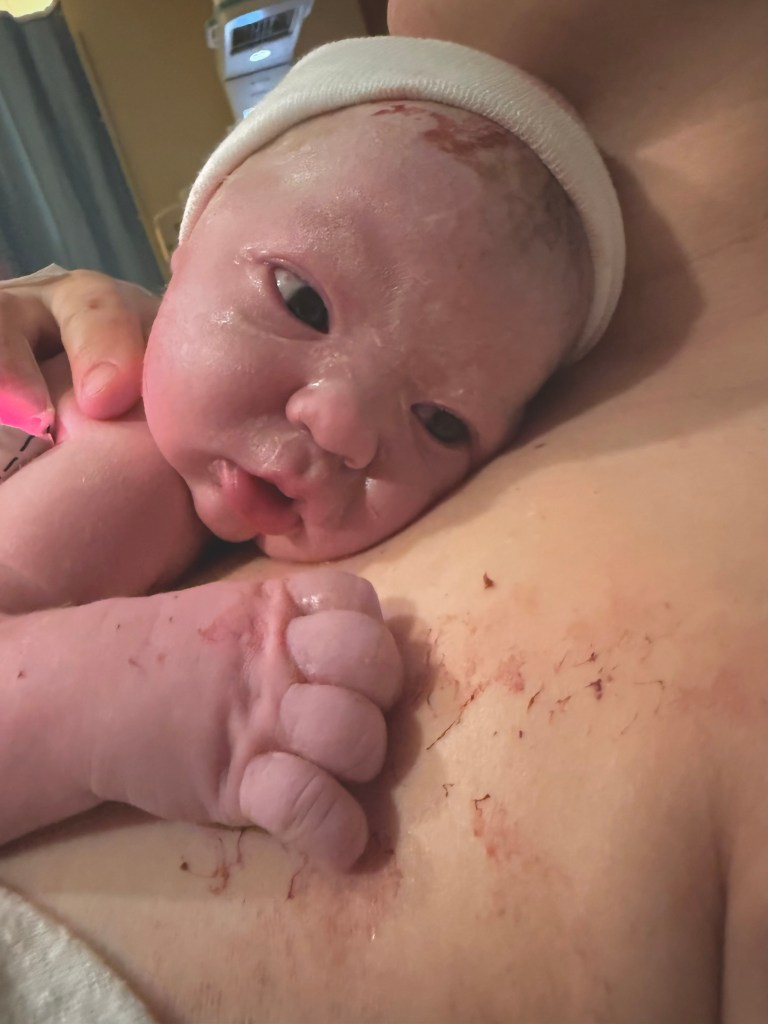
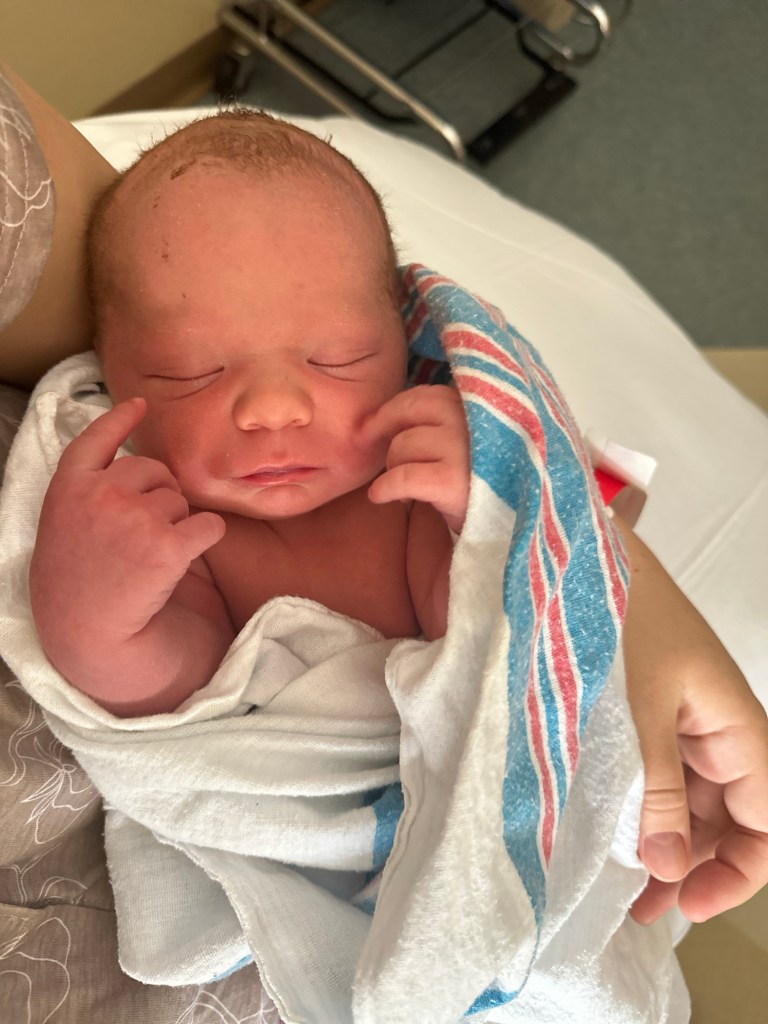
As our sweet almost one week old rests next to me in the BJORN getting some day light through the window, I wanted to sit down and start to type out his birth story. I’ve written birth stories down for all the kiddos and I’ve tried to do it as soon as possible while everything is so fresh.
I am 40 years old. To me, its just another number. I don’t feel 40, or look 40 (says everyone who finds out my age) and I probably don’t act 40. To the medical establishment it means advanced maternal age. Basically, when you’re 40 and pregnant, you’re a grandma in hospital age talk.
When I found out I was pregnant with our third child, Teddy, I knew I wanted to avoid a repeat c-section at all costs.
Having a vaginal birth with Emery and then a C-section with Archie left me in the unique position to compare the two. While both have their cons — recovering from a vaginal birth is so hard on the body, too, especially if you have tears (I did and do), hurt your tail bone (I did x2), had long labors (24 hours, 27 hours)…. and so on… vaginal births have some major pros. There is still nothing quite like knowing and feeling that you birthed your child vaginally, setting them up for health right from the get go. Not only does birthing vaginally help your babies gut and immune system immediately, but it even helps prevent developing allergies and asthma and other ailments. Lung function is improved, bonding and alertness is stronger and higher, and immune system development gets a kick start as babies body scoops up mama’s healthy flora as it descends the canal.
And then you have the risks of a c-section (WAY more risks associated with c-sections) & these risks get higher with each c-section. Then the recovery and long term implications of having your entire abdomen sliced open. I could go on and on. A simple google search leads to hundreds of articles on the benefits of vaginal births over c-sections. Thankfully we have modern medicine and necessary c-sections can save lives. But let’s be real – how many c-sections are ACTUALLY necessary? Shockingly around 70% of women are likely eligible for a TOLAC (trial of labor after cesarean) and would actually benefit from having one over a repeat c-section. Guess how many actually do a TOLAC? About 13%. That’s STARK. The reality is this, whether you feel triggered by this post or not, C-sections are money makers. They’re “easy” for the doc, and in many cases, they’re easy for the mom. Schedule the date. Show up. Baby is removed. Go on. I’ve had one. I know. When I became pregnant with Teddy my OB told me “We’ll schedule you for a delivery in the beginning of week 39” For many women, theirs is scheduled week 37. So they’re also taking babies before they reach full term, further setting them back. I could go on and on and on.
Finding a provider who is supportive of a VBAC is not always easy. In many places, hospitals won’t even consider them because they do not have anesthesiology at the hospital around the clock. So it definitely takes some work. Had we had stayed in Colorado I would have had to travel to the city — Denver or Boulder — to labor and deliver. There was no place within a couple of hours of me that was set up to accept a VBAC. There are risks with a VBAC, the most notable being uterine rupture. Basically, the scar from your c-section could open up, causing your baby to essentially fall into the abdominal cavity. This is a medical emergency and while rare, it can be life threatening to mom and baby and being taken to surgery immediately is key in a better outcome. After calculating my risk factors, my risk of uterine rupture going into my VBAC attempt was less than 1%
I found my provider in January. The hospital is about 7 minutes from our house. I ended up switching my provider, but staying at the same hospital, a few weeks before Teddy’s due date. My new provider, Dr. F, was amazing. Knowing my age and the overall increased risk of not only still birth but declining VBAC success rates after 40 weeks (due to various issues), she suggested I be induced on my due date. She suggested breaking my water, if I was dilated enough, and just going from there. It was understood that we would only begin Pitocin after allowing my body time to kick into labor on it’s own. I went back and forth on induction. Back and forth. Back. And. Forth. After two weeks of prodromal (false) labor, acupuncture, chiropractor, curb walking, a membrane sweep, etc. I was really thinking I’d go into the induction ready to have him.
Little did I know….
Teddy’s Birth Story : Successful VBAC
We arrived at the hospital late Monday night the 23rd of March.
11:40pm – Water broken by OB on Call. I was STILL only 2cm dilated after an intense weekend of painful contractions at times, membrane sweep, curb walking, rest, etc. I was also -2 Station. I told the doctor (who has NOT my regular OB) I wanted to ensure baby was at a safe station prior to her breaking my water. As she checked my dilation it was incredibly painful for me. In the middle of gasping for breaths I asked her if everything looked good to go and he was in a good station and she said yes. Note: -2 is not a good station for AROM (Artificial rupture of membranes). In fact, it actually puts you at risk of cord prolapse which can actually be deadly, quickly, to the fetus. For the next two hours Ben and I stressed out, big time. To that doctor, maybe that was okay, but to us and allllll of the hours of research I’d done and statistics, it wasn’t. So I started off my induction incredibly angry. Thankfully, the risk after a couple of hours is basically zero, and we were able to finally breathe a sigh of relief.
For the next 10 hours we “rested” (I didn’t sleep a wink), while my body tried to kick itself into labor. Sometime around 9am I decided I didn’t want to labor without medication. I kind of had a feeling going into Teddy’s birth that I was going to get an epidural. I just wasn’t feeling a natural birth attempt this time around. With Emery it was all I ever wanted, and I was devastated when the birth center kicked me out for laboring too long and had me go to the hospital for an epidural to help relax. So devastated, I cried. I just needed a few more hours. With Archie, I didn’t get the epidural until I was attempting to push him out at 9.5-10cm, and then shortly thereafter I was taken to surgery. This time I had already been awake for 24 hours, was emotionally and physically exhausted, and knew I didn’t want to labor all night and all day without pain management. I also knew it would help the immense amount of anxiety I was feeling having undergone an induction.
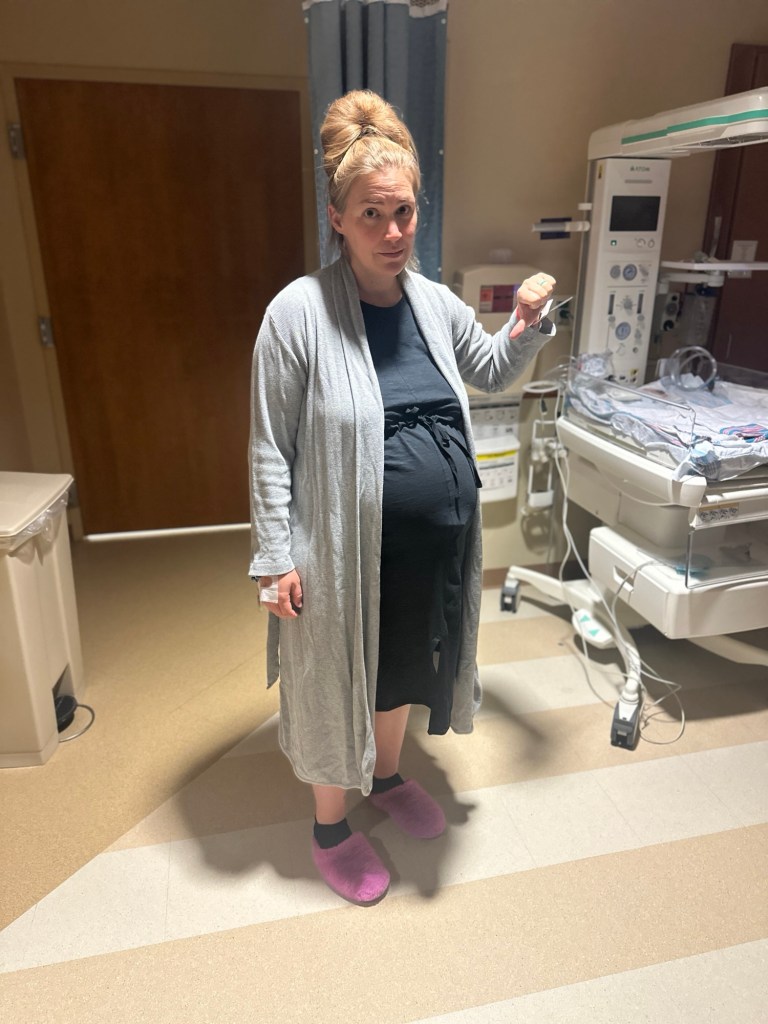
9am ish – Epidural placed
10:10am – After 11 hours I was only 3-4cm dilated, 80% effaced and baby was still high up at -2 station. The nurses asked me if I’d be okay with Dr. F ordering a low start rate of Pitocin. I agreed. Pitocin started at 2. (Too high of a dose of Pitocin is contraindicated in VBAC’s because of the increased risk of uterine rupture). Anything above 12-20 is controversial in a VBAC. In a regular vaginal, 30 is typically the max.
Around this time my blood pressure had a negative reaction to the epidural, and my BP was in the low 80’s. I was asked if I consented to a one time dose of Ephedrine to which I did. It helped.
11:20am – The nurses asked if I would consider the Pitocin being raised to 4. I gave consent.
11:55am – 6cm dilated. The pitocin was working!
Blood pressure issue continued. I received a 1000ml bolus of IV fluids and then sometime after another 500. I have low blood pressure at baseline, so this was not that surprising to me. My body reacts very strongly to pain medication.
12:35pm – I was feeling the epidural was too strong and I asked anesthesiology to turn it down. It was lowered from 12 to 8.
2:20pm – Once again I was feeling the epidural was too strong. I did not want to be completely numb from the waste down. I was also worried about its strength continuing to impact my BP and in turn, the baby. Epidural lowered from 8 to 4. It was barely on at this point.
3:00pm – Pitocin completely stopped due to baby having some heart deceleration’s at the end of contractions. These were super short lived, nothing too concerning for the doc, but even that tiny dose of pitocin was potentially having an impact. After it was stopped, contractions slowed WAY down.
3:25pm – Pitocin restarted low at 2. 7cm dilated! Slow and steady progress. Baby believed to be sunny side up, a poor position, causing me extra pain and stalling him from coming down the birth canal.
4:45pm – I was crying in pain. Having excruciating round ligament pain. I could breathe through the contractions and I was using a birth comb (highly recommend!) but I could not handle the round ligament tearing pain. It was too much for me. Epidural had completely warn off. Anesthesiology at bedside to discuss plan with me. Trying to find my happy medium between some pain relief & not being too numb.
Oxygen on now for a while to see if it helped with baby heart decelerations. Still not at a concerning number, but being cautious. Lowering or Upping the epidural had seemingly no impact positive or negative on the heart rate changes of the baby. His changes were related to 1. whenever I was on my left side to help open pelvis 2. pitocin even at the lowest dose possible.
5:15pm – 8cm dilated, baby has finally moved down just a little. -1 station
7:49pm 9cm, -1 station
10:00pm – Found a happy medium with the epidural for a bit. Round ligament tearing pain getting better. Could completely feel my legs and had ability to get on knees and lean over top of bed. Stayed this way for over an hour to help baby descend. It worked!
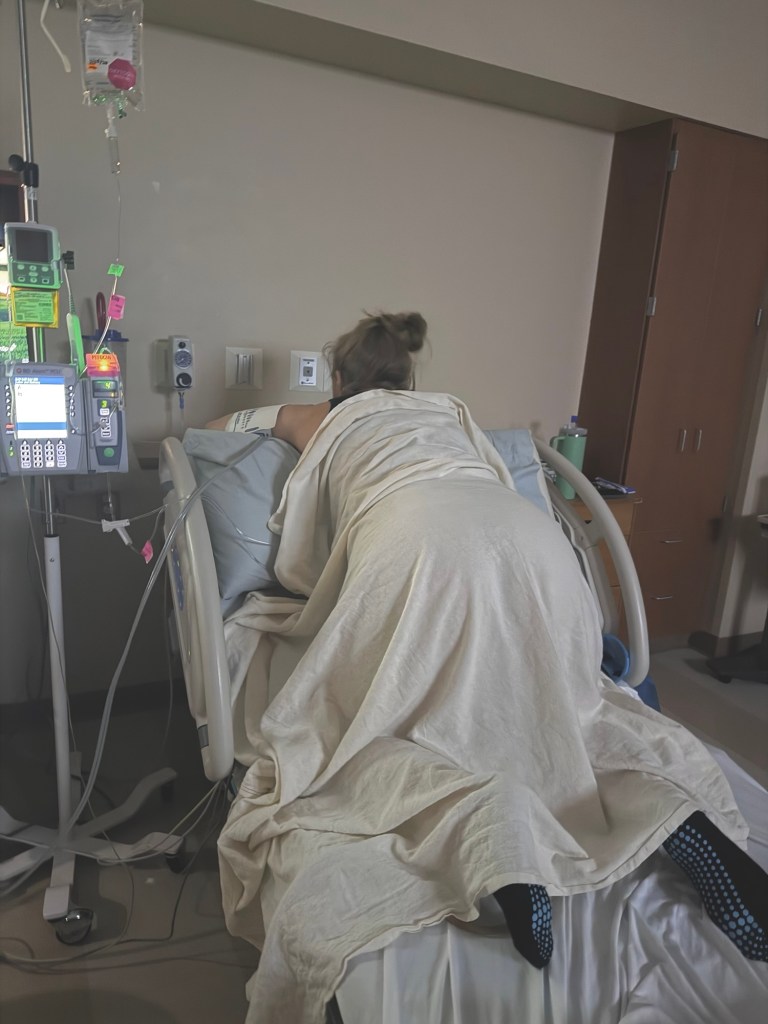
Epidural wore off again. Fun times!
12:00am March 25th – 10cm dilated, time to push
12:00 – 02:54am – Dr. F arrived to my room. There were 2-3 other babies being born at the same time! Time to have mine! Pushing while side lying, Ben holding my upper leg up to facilitate opening the pelvis. I refused to lie on my back. I also didn’t feel comfortable enough being on all fours because my epidural had worn off substantially, even with anesthesiology coming in multiple times to trouble shoot. I failed the entire epidural cold swab test (aka I could feel everything everywhere). Anesthesiology ended up turning it up. The issue wasn’t just the pain of the contractions…. for 10 hours now I had been having the excruciating round ligament pain off and on as if the ligament was being completely shredded during and after contractions. There was no relief. Because I was laboring on my right side, my left side where I was feeling the ligament stretching, was not numb at all due to the distribution of the epidural. This, along with back labor and epidural failure intermittently and position dependent = so much pain. I was also very discouraged at times that pushing was taking so long. I’d been up since 7am on the 23rd. 42+ hours…. Exhaustion was hitting hard. L and D nurses assured me there was no rush, baby and me were completely healthy, I’d have a baby soon, and to keep going. Ben, my doula Laura, L & D nurses, Dr. F — ALL were encouraging me and I am so thankful for them.
02:54am – Someone asked if I wanted to put my hand down and feel Teddy’s head coming out. I did. He was born shortly after. 4-5 final pushes and I felt him come out in his entirety followed by instant pain relief. He came out screaming! The cord was very tightly wrapped around his neck & quickly removed by Dr. F (Fact: Around 50% of babies are born vaginally with the cord wrapped around their neck). APGAR’s of 8 and 9. Our perfectly healthy baby boy!!!!
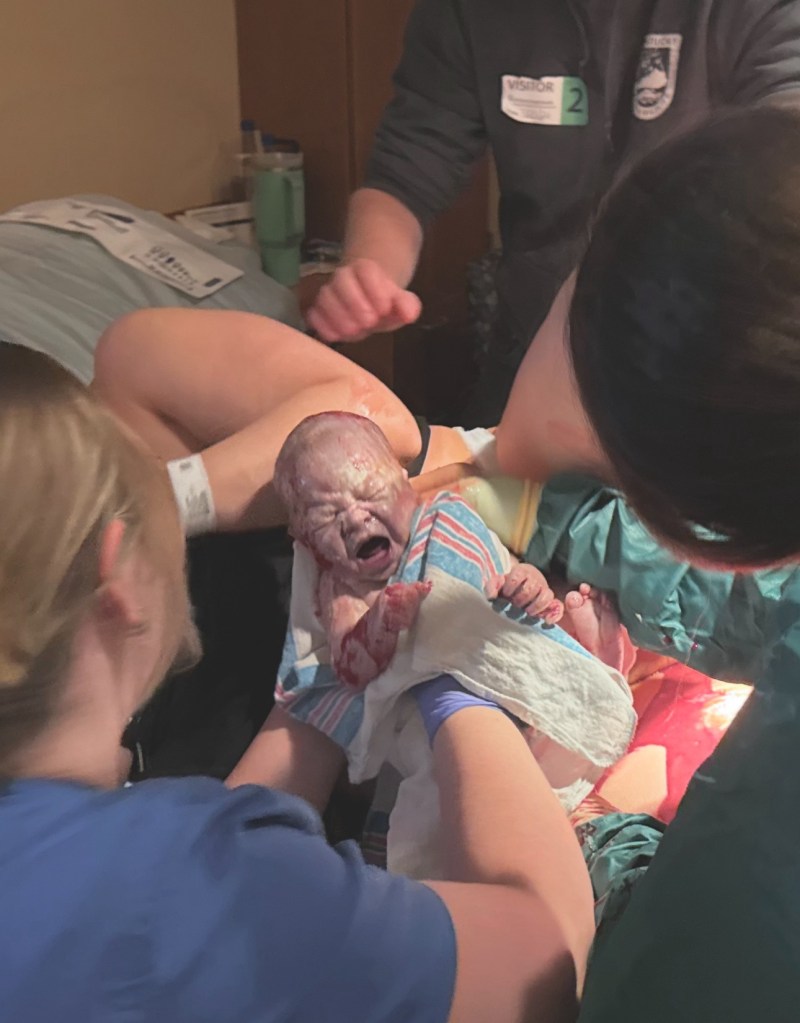
Immediately Post Birth
Teddy caught by doctor and immediately given to me with cord still attached and pulsating. After it stopped and turned completely white, Dr. F helped Dad cut the cord! Golden hour started. Golden hour x 2, actually. Just me holding my boy. I suffered a second degree tear so Dr. F stitched me up. Laura, my doula, was able to take pictures of the placenta and she showed us the sac attached to it. Healthy red placenta! Teddy latched on and nursed for the first time.

Me, Ben, Laura breathed many sighs of relief. Laura headed home some time after 4am. She’d been with me since 9am ish the day prior. Talk about a rock star doula. I can’t even explain what her presence did for me during the entire experience. 10/10
In Summary….
Regarding the induction — My body wasn’t ready and even though I was 40 weeks pregnant, it was my due date & I’d been having all of the signs of coming labor for two weeks, my body was not ready. Such is the case with many inductions. I could have waited until 40+3, 40+5, but having gone well past 41 weeks and having that end in a c-section with Archie, I was understandably nervous of that happening again. So I chose the induction. If I have a fourth baby, I will wait longer and potentially set my body up for more success (ie. a shorter labor).
Regarding the overall labor — My doula and nurses were absolute rock stars. The L and D nurses must have set a timer because every 30-45 minutes they were at my bedside helping me move into a new position. Peanut Ball. Pillows. Side lying release. You name it. They helped me get into that position. So thankful for these women who helped me tremendously.
Regarding the doctor — She never ONCE pressured me. Never. Once. My body and baby were allowed the long time they needed. My water had been broken for 27 hours total. 3 long hours of pushing. She said to me after “Girl I wasn’t going to interrupt! You were doing your thing! You did it!”
Overall — the best part of the experience for me was the support through labor. The worst part of the experience for me was the postpartum care. Horrible hospital food. Way too many vital signs checks on me and baby, no sleep, a million interruptions, a rude pediatrician….. we had to beg to get out of the hospital on the 26th. I was NOT staying another night.
One week ago today I was in full labor. Today I’m at home recovering with a sore tail bone and a healthy baby. I’m not recovering from a c-section. I had a successful VBAC. I am so, so, so thankful. Induction, epidural, and all. So thankful. So relieved.
Every one of my birth stories is so different. Despite the immense amount of pain I was in for Teddys birth, the sobbing that came with the hormone rush of transition, and the overwhelming fear I sometimes felt — there is nothing like feeling those final contractions and actually feeling your body birth a baby during those final pushes. I will never forget that feeling. I am so thankful my epidural only worked sometimes. Even if I was crying hysterically during those times 😂